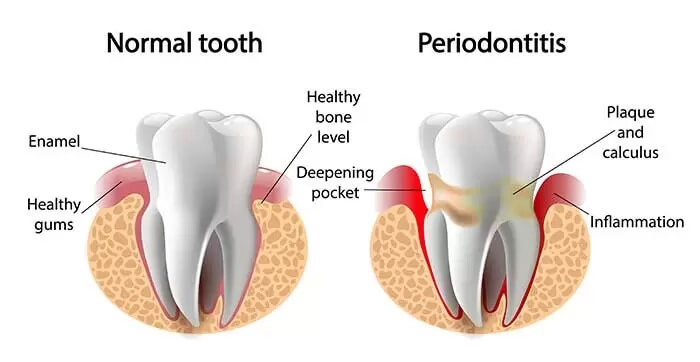
What Is Periodontitis?
When left untreated, gingivitis can lead to the development of a more serious form of periodontal disease, periodontitis. Over time, bacterial plaque can spread and grow below the gum line and calcify to form calculus (tartar). Bacterial toxins emitted from the plaque irritate the gums.
The toxins stimulate the immune system to create a chronic inflammatory response. Essentially, during the chronic inflammatory response, the body turns on itself, breaking down and destroying the tissues and bone that support the teeth. By this point, gums begin to separate from the teeth, forming periodontal pockets (spaces between gums and teeth) that become infected with periodontal pathogens.
As the disease progresses, more gum becomes infected, the bone is destroyed down the length of the tooth and the periodontal pockets deepen. Often, this destructive process has little to no symptoms. Eventually, the patient becomes aware something is wrong when teeth begin to shift or become loose. By this point, if the disease has severely affected the bone, the teeth may have to be removed.
What Are The Signs And Symptoms Of Periodontitis?
Some symptoms of Periodontitis include:
- Inflamed (swollen) gums
- Gums are fiery red, sometimes purple
- Gums are tender or hurt to touch
- Gum recession, making teeth look longer
- Extra spaces appear between the teeth, teeth shifting
- Pus may appear between the teeth and gums
- Bleeding when brushing, flossing or eating
- Halitosis (bad breath) that won’t go away
- Loose teeth
- Sore in the mouth
- A change in partial denture fit
- A change in the bite
Are You In Need Of A Periodontist In Jupiter?
If you are suffering from periodontitis, refer to our treatment page for more information on treatment options, or, call our office to schedule your consultation today! Dr. Fotek and our team of skilled professionals are committed to helping you achieve a beautiful, healthy smile with gentle periodontal treatment, implant dentistry, and preventative care.
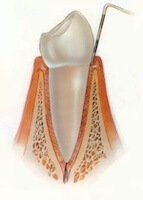
Gums of pink and firm with no sign of bleeding
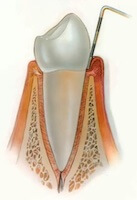
Gums are slightly reddish and may be swollen, bleeding while brushing and flossing.
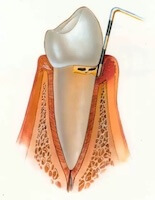
Initial bone loss observed, gums are puffy and begin to separated from the teeth. Gums bleed easily.
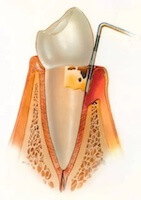
Gums begin to recede, puffy and bleed easily. Some teeth begin to be slightly loose.
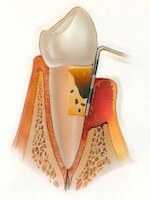
Gums are puffy, bleed spontaneously with evidence of pus oozing from the pocket. Teeth may be very loose due to bone loss.

